PHILIPE DE SOUTO BARRETO1,2
1. Gerontopole of Toulouse, Institute of Ageing, Toulouse University Hospital (CHU Toulouse), Toulouse, France; 2. UPS/Inserm UMR1027, University of Toulouse III, Toulouse, France.
Corresponding to: Dr. Philipe de Souto Barreto, Gérontopôle de Toulouse, Institut du Vieillissement, 37 Allées Jules Guesde, F-31000 Toulouse, France, Phone: (+33) 561 145 668, Fax: (+33) 561 145 640 e-mail: philipebarreto81@yahoo.com.br
Care Weekly 2018;2:4-8
Published online November 5, 2018, http://dx.doi.org/10.14283/cw.2018.6
Abstract
Physical activity (PA) and exercise have been found to be associated with a reduced risk of developing major adverse health events during aging without important side effects. However, PA and exercise counselling in routine clinical care is still rare, particularly in the primary care. This opinion paper synthetizes the scientific evidence on the benefits of PA and exercise during aging in order to guide practitioners to advise/prescribe this healthy behavior. Guidance for sitting time is also provided. A specific focus is performed in a population at particular risk for short-, medium and long-term adverse events: middle-aged adults with obesity. In conclusion, all healthy patients (with or without diseases/conditions) may safely increase their PA levels and exercise. Stratifying patients according to the potential benefits they may obtain from PA and exercise counselling may help health practitioners to optimize their care approach by spending the “right time” with the “right person”.
Key words: Physical activity, exercise, elderly, routine care.
Introduction
Physical activity (PA), roughly defined as any body movement in any PA domain (such as, leisure-time, housework, occupational, and commuting) performed through muscle contraction with associated energy expenditure, has been extensively found to be associated with a reduced risk of developing major adverse health events during aging, including mortality, several non-communicable diseases, such as diabetes, cardiovascular diseases, some types of cancer, cognitive decline and Alzheimer’s disease (1–4). Exercise, a subtype of PA which is structured, repetitive and purposeful, has found to positively impact major clinical outcomes, such as mobility disability, overall falls and injurious falls,(5–7) and is often used as a complimentary therapeutic instrument in the treatment of various diseases(8).
Despite the striking scientific evidence supporting PA and exercise health benefits during aging, the translation of these research findings into clinical care is a challenge difficult to overcome. If we take the example of primary care practitioners, we observe that PA is almost never mentioned during consultations (9–12). When this health behavior is mentioned, time spent discussing on it is extremely short, rendering it impossible to provide useful guidance to patients (13,14). Although lack of time is one of the most important barriers for health professionals to advise their patients on PA and exercise(14), other two obstacles are important to mention: lack of knowledge by health professionals on PA and exercise recommendations and lack of precise evidence-based protocols, especially for multimorbid (ie, people with two or more diseases) patients who constitute a high fraction of older adults. Another potential issue is the population(s) to be targeted in priority for a more in-depth counselling: indeed, PA and exercise have the potential to benefit health of almost all patients, but some people are more in need of PA/exercise-induced health improvements than others.
The objective of this opinion paper is to synthetize the scientific evidence on the benefits of PA and exercise for older adults in order to guide practitioners to advise/prescribe this healthy behavior in routine clinical care.
What should I prescribe and for whom?
The majority of patients may benefit from a physically active behavior during aging. However, patients with any unstable condition (ie, presenting signs and symptoms(15)) that could be negatively affected by PA and exercise should be referred to the appropriate specialist for a thorough clinical examination and, if the specialty physician allow them to exercise, they may need to exercise under the supervision of an exercise expert (eg, clinical exercise physiologist). Another population that may require further attention and exercise under supervision is composed of people at increased risk of falling: studies have shown that, for example, very old (≥ 80 years) individuals, recently hospitalized, most of them having recently fallen (eg, in the last 12 months), have a higher risk of falling due to exercise (16).
Overall healthy patients (including those with stable/asymptomatic clinical conditions) may safely benefit from PA and exercise, which constitute a powerful instrument of health promotion with only minor “side effects” (eg, muscular-skeletal soreness). There are different levels of counselling according to patients characteristics and needs, going from simple and short PA advices to a precise exercise prescription (in terms of exercise type, duration, frequency, and intensity).
Patients without chronic diseases or clinical conditions
Disease- and clinical condition-free patients may be advised on the basis of the current public health guidelines on PA (17), with small adaptations. Current recommendations (17) indicate that adults and older adults should do at least: 150 min/week of moderate aerobic PA or 75 min/week of vigorous aerobic PA or an equivalent mix of moderate and vigorous PA AND ≥ two days/week of muscle strengthening activities AND ≥ three days/week of balance activities; recommendations on balance apply only to older adults with mobility limitations. Although stimulating patients to reach these guidelines may constitute a goal, the most important information that should drive counselling on PA in clinical care should be: doing some PA is better than nothing, doing more is better than some, whatever the amount of PA you do you will get some health benefits. This message is essential and is fully based on scientific evidence: it is well-known that the PA-health association is dose dependent (18–22) and that the highest health gains occur when sedentary people start doing some PA (4, 21). When adapting the above mentioned guidelines, healthcare practitioners should focus on PA related to the domains of leisure-time (eg, sports, exercise, hiking, playing with grand-children) and commuting (going from one place to another by walking briskly or cycling) (23) and stimulate patients to start and progress slowly (do not struggle to make people doing 150min/week immediately; instead ask people to make 10 minutes of moderate PA in a day, which may represent, for example, a round-trip of brisk walking to buy groceries near to their home). Regarding strength, simple weight-bearing activities may be advised, such as raising from a chair several times or climbing stairs. Regarding suggested balance activities for older people with mobility limitations, the best approach is to refer these patients to an exercise specialist since they may represent a population at increased risk of falling (in particular in the first weeks of increasing PA) if they exercise without supervision.
Patients with asymptomatic chronic disease or clinical conditions
Patients with one or more asymptomatic chronic diseases and clinical conditions may also benefit from PA and exercise. The same overall message used for disease-free patients applies to people with chronic conditions, ie, move your body somewhat even if you do not achieve PA guidelines. However, these patients may need a structured exercise training as a complimentary therapeutic approach in order to facilitate the management of disease’s signs and symptoms. There are disease-specific, evidence-based exercise protocols for some of the most prevalent conditions (eg, hypertension, cardiac disease, diabetes, obesity, depression, low back pain) observed in the primary care (8); such protocols have been developed and/or ratified by the disease-specific learned/scientific societies. The issue that may arise is that older people are often suffering from and being treated for more than one disease/condition; in such a case, what exercise protocol should be privileged for multimorbid people?
As I have discussed in a previous publication (8), the good news is that most disease-specific exercise protocols provide a very similar exercise structure, which may mean that a single exercise prescription could fit for several multimorbid patients. In overall, asymptomatic patients, including multimorbid subjects, should be advised to perform: a total of 90min/week or over of aerobic (ie, any cyclic activity) exercises (eg, brisk walking, jogging, cycling, sports), in three or more days/week AND twice/week of strength exercises (eg, chair rises, stair climbing, but also weight lifting or functional training in a fitness center). Aerobic and strength exercises may be performed in the same day and even during the same exercise session. All exercises should be performed in, at least, a moderate intensity, which roughly means they should be physically demanding and should not lead to disproportionate breathlessness and exhaustion: moderate-to-vigorous intensity corresponds to a perceived exertion rate of 5 to 7 on a 10-point scale (0 is sitting and 10 is the maximum effort possible) for aerobic exercises and being able to properly perform between 8 and 15 repetitions for strength exercises.
The sitting issue
Although international public health PA guidelines as well as national PA recommendations in most countries provide no guidance on sedentary time, literature in the past 10 years has shown that sitting time (in particular, TV viewing time) is a major risk factor for the onset of cardiometabolic diseases and mortality (24–26). The harmonized meta-analysis by Ekelund et al. (26) found that both sitting for longer than 4hr/day and TV viewing for 3hr/day or over were associated with increased mortality; such association was mostly independent of PA levels, being counterbalanced by a physically active lifestyle only in very active people (those doing > 35.5hr-MET/week, which corresponds to approximately 100min/day, 5 days/week of brisk walking – what corresponds to more than three times the current minimum recommendations on PA). This suggests that the detrimental effects of sedentary time is independent of PA levels for the large majority of the population. Therefore, healthy patients should be advised to restrict usual sitting to <4hr/day preferentially, and no longer than 7hr/day. Breaking the time spent seated has shown to improve metabolic parameters (27, 28) and should be encouraged; although no precise “breaking sitting time” protocol exists, counselling people to spend 2-to-5 minutes in at least light-intensity activities, such as walking, after each hour of sitting might be feasible for most of them and should be emphasized. This is of particular importance for middle-aged people who works in seated positions all day long.
The obesity in middle-aged patients: a high priority population
Obesity, defined as body mass index ≥30kg/m², in midlife (from about 40-45 years to 60-65) is associated with a myriad of adverse events, in the short and long-term, including early mortality, cardiovascular diseases, diabetes, Alzheimer’s disease and other dementias, and the incidence and worsening of disability in both basic and instrumental activities of daily living (29–34). Although individuals with obesity should be systematically advised for performing PA and exercise (preferentially between 150 and 300 min/week), it is important to highlight that the obesity issue can only be tackled by a multidimensional strategy involving PA and exercise, but also nutrition and potentially other contributing elements (eg, social support).
How to proceed in a clinical care consultation?
Pragmatically, the best approach to advise people on PA or prescribe an exercise protocol in clinical care is to use the 6As’ strategy (35): assess, advise, agree, assist, arrange, and assess again. Having a global clinical examination, including a comprehensive geriatric assessment for older adult patients, is important to establish the most precise and adapted exercise program, which will have the highest chance to be effective to the patient. However, this is rarely the case for busy primary care practitioners. An alternative to 6As and comprehensive clinical examination might be the single standardized prescription for healthy individuals (including people with asymptomatic diseases/conditions), as I have previously suggested in the context of multimorbidity (8).
Three questions are indispensable when health practitioners intend to advise their patients (8): how many days in a typical week do you undertake moderate or vigorous PA (example, cycling or walking briskly, jogging) during your leisure-time or for transportation purposes? On each of these days, how many minutes do you spend doing such activities? How many hours do you spend in sitting position (eg, for viewing TV, reading) in a typical day? Disease- or clinical condition-free patients indicating to engage in less than 30 min/week of PA, as well as those with a clinical condition for which exercise is recommended and who do less than 60min/week might constitute the main target populations; a larger consultation time may be needed for these patients in order to explain the importance and arrange a progressive raising of PA levels or for prescribing an adapted exercise protocol. All patients indicating to spend > 4hr/day sitting, in particular those spending >7hr/day, should be advised to reduce their sitting time and/or to break sitting time with light walking or an equivalent activity. Providing patients with written materials and even a formal prescription (similar to a drug prescription) may be crucial (see an example in De Souto Barreto (8)). Figure 1 displays the flow of procedures for counselling patients about PA, exercise and sitting time in the clinical setting. Box 1 presents a summary of counselling/prescription main elements.
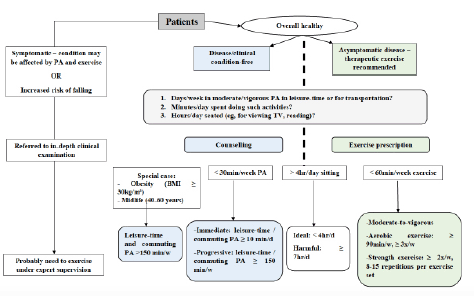
Figure 1: Flow of procedures and patients for counselling/prescribing physical activity/exercise in routine clinical care

Box 1. Overall guidance for physical activity counselling and exercise prescription in routine clinical care.
Conclusion
In sum, all healthy patients (with or without diseases/conditions) may safely increase their PA levels and exercise slowly and progressively (for example, increasing exercise frequency, duration and/or intensity). The most vulnerable individuals, who are in overall sedentary people aged ≥ 80, should be advised to exercise up to three times a week (higher weekly frequencies possibly augmenting the risk of falling).
Different patients, with different levels of risk factors for adverse events, require different levels of information in terms of PA and exercise to improve this healthy behavior. Focusing on those who may mostly benefit from PA and exercise, such as sedentary people with risk factors for adverse outcomes and who spend too much time seated, may help health practitioners to spend the “right time” with the “right person” in their routine clinical care.
Conflict of Interest
None
References
1. GBD 2015 Risk Factors Collaborators. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Lond Engl. 8 oct 2016;388(10053):1659‑724.
2. Lee I-M, Shiroma EJ, Lobelo F, Puska P, Blair SN, Katzmarzyk PT, et al. Effect of physical inactivity on major non-communicable diseases worldwide: an analysis of burden of disease and life expectancy. Lancet Lond Engl. 21 juill 2012;380(9838):219‑29.
3. Norton S, Matthews FE, Barnes DE, Yaffe K, Brayne C. Potential for primary prevention of Alzheimer’s disease: an analysis of population-based data. Lancet Neurol. août 2014;13(8):788‑94.
4. Warburton DE, Charlesworth S, Ivey A, Nettlefold L, Bredin SS. A systematic review of the evidence for Canada’s Physical Activity Guidelines for Adults. Int J Behav Nutr Phys Act. 11 mai 2010;7:39.
5. Pahor M, Guralnik JM, Ambrosius WT, Blair S, Bonds DE, Church TS, et al. Effect of structured physical activity on prevention of major mobility disability in older adults: the LIFE study randomized clinical trial. JAMA. 18 juin 2014;311(23):2387‑96.
6. Guirguis-Blake JM, Michael YL, Perdue LA, Coppola EL, Beil TL. Interventions to Prevent Falls in Older Adults: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA. 24 2018;319(16):1705‑16.
7. Tricco AC, Thomas SM, Veroniki AA, Hamid JS, Cogo E, Strifler L, et al. Comparisons of Interventions for Preventing Falls in Older Adults: A Systematic Review and Meta-analysis. JAMA. 07 2017;318(17):1687‑99.
8. de Souto Barreto P. Exercise for Multimorbid Patients in Primary Care: One Prescription for All? Sports Med Auckl NZ. 6 avr 2017;
9. Smith AW, Borowski LA, Liu B, Galuska DA, Signore C, Klabunde C, et al. U.S. primary care physicians’ diet-, physical activity-, and weight-related care of adult patients. Am J Prev Med. juill 2011;41(1):33‑42.
10. Bock C, Diehm C, Schneider S. Physical activity promotion in primary health care: results from a German physician survey. Eur J Gen Pract. juin 2012;18(2):86‑91.
11. van Dillen SME, Noordman J, van Dulmen S, Hiddink GJ. Examining the content of weight, nutrition and physical activity advices provided by Dutch practice nurses in primary care: analysis of videotaped consultations. Eur J Clin Nutr. janv 2014;68(1):50‑6.
12. Galaviz KI, Jauregui-Ulloa E, Fabrigar LR, Latimer-Cheung A, Lopez y Taylor J, Lévesque L. Physical activity prescription among Mexican physicians: a structural equation analysis of the theory of planned behaviour. Int J Clin Pract. mars 2015;69(3):375‑83.
13. Bardach SH, Schoenberg NE. The content of diet and physical activity consultations with older adults in primary care. Patient Educ Couns. juin 2014;95(3):319‑24.
14. Hébert ET, Caughy MO, Shuval K. Primary care providers’ perceptions of physical activity counselling in a clinical setting: a systematic review. Br J Sports Med. juill 2012;46(9):625‑31.
15. Fletcher GF, Ades PA, Kligfield P, Arena R, Balady GJ, Bittner VA, et al. Exercise standards for testing and training: a scientific statement from the American Heart Association. Circulation. 20 août 2013;128(8):873‑934.
16. Sherrington C, Lord SR, Vogler CM, Close JCT, Howard K, Dean CM, et al. A post-hospital home exercise program improved mobility but increased falls in older people: a randomised controlled trial. PloS One. 2014;9(9):e104412.
17. World Health Organization. Global recommendations on physical activity for health. WHO Press; Geneva, Switzerland: p. 58; 2010.
18. Arem H, Moore SC, Patel A, Hartge P, Berrington de Gonzalez A, Visvanathan K, et al. Leisure time physical activity and mortality: a detailed pooled analysis of the dose-response relationship. JAMA Intern Med. juin 2015;175(6):959‑67.
19. de Souto Barreto P, Cesari M, Andrieu S, Vellas B, Rolland Y. Physical Activity and Incident Chronic Diseases: A Longitudinal Observational Study in 16 European Countries. Am J Prev Med. 13 oct 2016;
20. de Souto Barreto P, Delrieu J, Andrieu S, Vellas B, Rolland Y. Physical Activity and Cognitive Function in Middle-Aged and Older Adults: An Analysis of 104,909 People From 20 Countries. Mayo Clin Proc. nov 2016;91(11):1515‑24.
21. Moore SC, Patel AV, Matthews CE, Berrington de Gonzalez A, Park Y, Katki HA, et al. Leisure time physical activity of moderate to vigorous intensity and mortality: a large pooled cohort analysis. PLoS Med. 2012;9(11):e1001335.
22. Moore SC, Lee I-M, Weiderpass E, Campbell PT, Sampson JN, Kitahara CM, et al. Association of Leisure-Time Physical Activity With Risk of 26 Types of Cancer in 1.44 Million Adults. JAMA Intern Med. 1 juin 2016;176(6):816‑25.
23. de Souto Barreto P. Time to challenge public health guidelines on physical activity. Sports Med Auckl NZ. juin 2015;45(6):769‑73.
24. Grøntved A, Hu FB. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: a meta-analysis. JAMA. 15 juin 2011;305(23):2448‑55.
25. Chau JY, Grunseit AC, Chey T, Stamatakis E, Brown WJ, Matthews CE, et al. Daily sitting time and all-cause mortality: a meta-analysis. PloS One. 2013;8(11):e80000.
26. Ekelund U, Steene-Johannessen J, Brown WJ, Fagerland MW, Owen N, Powell KE, et al. Does physical activity attenuate, or even eliminate, the detrimental association of sitting time with mortality? A harmonised meta-analysis of data from more than 1 million men and women. Lancet Lond Engl. 24 sept 2016;388(10051):1302‑10.
27. Benatti FB, Ried-Larsen M. The Effects of Breaking up Prolonged Sitting Time: A Review of Experimental Studies. Med Sci Sports Exerc. oct 2015;47(10):2053‑61.
28. Duvivier BMFM, Schaper NC, Hesselink MKC, van Kan L, Stienen N, Winkens B, et al. Breaking sitting with light activities vs structured exercise: a randomised crossover study demonstrating benefits for glycaemic control and insulin sensitivity in type 2 diabetes. Diabetologia. 2017;60(3):490‑8.
29. Global BMI Mortality Collaboration null, Di Angelantonio E, Bhupathiraju S, Wormser D, Gao P, Kaptoge S, et al. Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet Lond Engl. 20 2016;388(10046):776‑86.
30. Winter JE, MacInnis RJ, Wattanapenpaiboon N, Nowson CA. BMI and all-cause mortality in older adults: a meta-analysis. Am J Clin Nutr. avr 2014;99(4):875‑90.
31. Al Snih S, Ottenbacher KJ, Markides KS, Kuo Y-F, Eschbach K, Goodwin JS. The effect of obesity on disability vs mortality in older Americans. Arch Intern Med. 23 avr 2007;167(8):774‑80.
32. Wee CC, Huskey KW, Ngo LH, Fowler-Brown A, Leveille SG, Mittlemen MA, et al. Obesity, race, and risk for death or functional decline among Medicare beneficiaries: a cohort study. Ann Intern Med. 17 mai 2011;154(10):645‑55.
33. Alzheimer’s Association. 2016 Alzheimer’s disease facts and figures. Alzheimers Dement J Alzheimers Assoc. avr 2016;12(4):459‑509.
34. Guh DP, Zhang W, Bansback N, Amarsi Z, Birmingham CL, Anis AH. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health. 25 mars 2009;9:88.
35. Khan KM, Weiler R, Blair SN. Prescribing exercise in primary care. BMJ. 2011;343:d4141.
